About Plantar Fasciitis
Your plantar fascia is the thick band of tissue that runs from your heel to your toes. If you develop plantar fasciitis, these tissues become inflamed. In other, more severe cases, tiny tears may develop in the fascia.
Is heel pain stopping you from doing activities you love? Do you wake up in the morning with a stinging pain in your foot? Plantar fasciitis is one of the most common causes of foot and heel pain, but it can be easily treated.

The Symptoms of Plantar Fasciitis
The first symptom of plantar fasciitis is typically mild heel pain, especially after exercising. As the condition worsens, the pain worsens, and more symptoms arise.
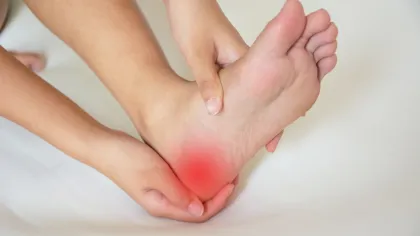
Stabbing Pain
Many people suffering from plantar fasciitis will feel a stabbing pain near their heels. This pain is typically worse right when you get out of bed in the morning or after you have been sitting for a long period of time.

Pain After Exercising
You will notice mild pain after exercising. As the condition advances, the pain will grow worse and can turn into stabbing or stinging pain.

Stiffness, Tenderness, and Swelling
As plantar fasciitis continues to go untreated, you will start to notice stiffness, tenderness, and even swelling. This is especially true in the mornings or after long periods of sitting.
Activities to Do at Home to Prevent or Alleviate Plantar Fasciitis Symptoms
Whether you are receiving non-invasive treatment, no treatment at all, or if you just finished your recovery from surgery, there are things you can do at home to help you prevent plantar fasciitis symptoms:

Stretch
Stretching is the most effective non-invasive treatment of plantar fasciitis. Continuing to stretch your calf muscles, foot, and ankle can help prevent plantar fasciitis from developing or worsening.

Take a Break
If you have more pain while performing a particular activity, take a break from that activity to give your plantar fascia time to heal. Switch out running with a low-impact exercise like swimming until you no longer have pain.

Ice
While this doesn't fix the problem, ice can help keep the inflammation down. If you are starting to have heel pain, try icing your foot for 20 minutes four times a day. Keeping the swelling down is important for your plantar fascia to heal.

Arch Support
Continuing to wear arch supports that are specific to your foot is important in preventing plantar fasciitis from recurring. Having proper support for your arch alleviates tension in your plantar fascia. This is especially important for people who have high arches or flat feet.
The Causes of Plantar Fasciitis
Plantar fasciitis is most likely to affect women between the ages of 40 and 60. However, other factors can increase your risk for developing this condition:
High Impact Exercises: Exercises that cause repetitive impacts on your feet, such as running or dancing, put added strain on your plantar fascia.
Obesity: Being overweight or having a sudden increase in weight, such as pregnancy, puts added stress on your plantar fascia.
High Arches or Flat Feet: Extremely high or flat arches put added stress on your plantar fascia.
Footwear: Wearing shoes with little to no arch support, especially when you already have high or flat arches, can damage your plantar fascia over time.
Career: Careers that require you to be on your feet for extended periods can put added stress on your plantar fascia and can even cause micro-tears.

Non-surgical Treatments for Plantar Fasciitis
Plantar fasciitis is a highly treatable condition. In most cases, you can make a full recovery with non-invasive therapies.
Physical Therapy
Stretching is the most common treatment for plantar fasciitis. Your physical therapist will work with you to stretch your plantar fascia, calf muscles, and Achilles tendon to help reduce the tension that is causing you pain. We work with several outstanding physical therapists who can prescribe an exercise regimen that is specific to you and your discomfort. Often, we will combine physical therapy with other treatment methods.
Night Splints
A night splint will stretch your calf muscles, Achilles tendon, and plantar fascia while you sleep. The night splint is a great addition to physical therapy as it continues to gently and effortlessly stretch the plantar fascia at home.
Orthotics
Orthotics are specially made inserts for your shoes. Your physician will take into account whether you have high arches or flat feet when prescribing your orthotics. These inserts are used to redistribute pressure on your feet, add arch support, and ease any inflammation of your plantar fascia.
Steroids
A steroid injection may be used to alleviate severe inflammation or pain. We will typically administer only one injection as multiple rounds can weaken or damage your plantar fascia.
Am I a good candidate for plantar fasciitis release surgery?
Surgery is considered a last resort, but sometimes it can be necessary. You may be a good candidate for this surgery if:
You still suffer from chronic foot and heel pain after trying other non-invasive methods.
Your pain has lasted for over six months while trying other, more conservative treatments.
Your pain is affecting your ability to perform daily activities and exercises.
Your pain is affecting the way you walk.
Your pain is interfering with your ability to work.
You do not suffer from underlying health issues such as diabetes.
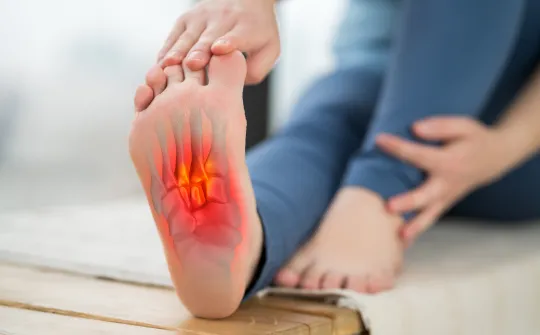

Plantar Fasciitis Release Surgery What to Expect
If we have tried everything else and you still suffer from chronic pain, we can perform plantar fasciitis release surgery to alleviate your symptoms.
If you are undergoing open surgery, you will be given general anesthesia to ensure you are unconscious throughout the procedure. Endoscopic surgery can be done with a local anesthetic and sedative.
During open surgery, your surgeon will make a 1-2 inch incision either along the bottom or back of your heel. During endoscopic surgery, your surgeon will make two incisions, each under half an inch, under your ankle bone.
During open surgery, your surgeon will detach your plantar fascia from your heel bone. If you have any spurs or trapped nerves, they can be removed at any time. During endoscopic surgery, your surgeon will insert a small lighted camera so they can view the treatment area. The camera is inserted into one of the openings while a scalpel is inserted in the other to detach the plantar fascia.
Both types of surgeries are outpatient. Your incisions will be sutured, and you'll be released when you are fully awake and your vitals have been checked. You will need someone who can drive you to and from your procedure no matter which type of surgery you had.
Surgery Aftercare
Your post-op instructions will depend on which type of surgery you had. For both types, your doctor may prescribe you pain medications or recommend over-the-counter meds.
Open Surgery Recovery
You may be required to wear a special shoe or walking boot for several weeks after your surgery. This helps your foot stay protected while it heals and alleviates the weight from walking. You will have a small scar where the 1-2 inch incision was made after the sutures are removed. You can begin wearing normal shoes when your doctor gives the ok, but full recovery typically takes between 6-10 weeks.
Endoscopic Surgery Recovery
This type has a quicker recovery period and you should be able to bear limited weight almost immediately after surgery. Rather than being put in a cast or a boot, you can wear regular shoes within 1-2 days post-operation. Since the incisions are less than half an inch long, your scars will be very small. You'll be advised on what activities to avoid following your surgery, but full recovery typically only takes between 3-6 weeks.
Heel Spur vs. Plantar Fasciitis
Heel spurs and plantar fasciitis can be difficult to tell apart. Both cause pain in the same area, so it is important to get your heel pain checked by a board-certified orthopaedic doctor.
Heel Spurs
Heel spurs are calcified deposits that grow on your heel. They are often painless, but when they do cause pain, it is similar to plantar fasciitis. A heel spur can extend as much as half an inch forward, but it is not visible to the naked eye, so x-rays are required to make a diagnosis.
Plantar Fasciitis
Your plantar fascia runs underneath where heel spurs tend to grow, which is why the cause of your pain can be confused. A diagnosis of plantar fasciitis is usually done through a physical exam and discussion of medical and occupational history. However, x-rays may be taken to rule out other causes.
What Our Patients Say





Dr. Seade did an excellent job on my torn rotator cuff repair! He also had to remove a bone spur and reattach my bicep muscle! My recovery has went very well and after 12 weeks I finally get to start strength training on my left shoulder and arm! I will be back barrel racing in no time!
LeAnn N.