Plantar fasciitis is a highly treatable condition. In most cases, you can make a full recovery with non-invasive therapies.

Plantar Fasciitis
About Plantar Fasciitis
Your plantar fascia is the thick band of tissue that runs from your heel to your toes. If you develop plantar fasciitis, these tissues become inflamed. In other, more severe cases, tiny tears may develop in the fascia.
Is heel pain stopping you from doing activities you love? Do you wake up in the morning with a stinging pain in your foot? Plantar fasciitis is one of the most common causes of foot and heel pain, but it can be easily treated.

The Symptoms of Plantar Fasciitis
The first symptom of plantar fasciitis is typically mild heel pain, especially after exercising. As the condition worsens, the pain worsens, and more symptoms arise.
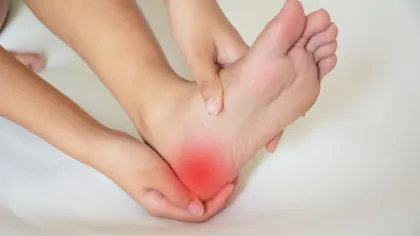
Stabbing Pain
Many people suffering from plantar fasciitis will feel a stabbing pain near their heels. This pain is typically worse right when you get out of bed in the morning or after you have been sitting for a long period of time.

Pain After Exercising
You will notice mild pain after exercising. As the condition advances, the pain will grow worse and can turn into stabbing or stinging pain.

Stiffness, Tenderness, and Swelling
As plantar fasciitis continues to go untreated, you will start to notice stiffness, tenderness, and even swelling. This is especially true in the mornings or after long periods of sitting.
Activities to Do at Home to Prevent or
Alleviate Plantar Fasciitis Symptoms

Stretch

Take a Break

Ice

Arch Support
The Causes of Plantar Fasciitis
Plantar fasciitis is most likely to affect women between the ages of 40 and 60. However, other factors can increase your risk for developing this condition:
- High Impact Exercises: Exercises that cause repetitive impacts on your feet, such as running or dancing, put added strain on your plantar fascia.
- Obesity: Being overweight or having a sudden increase in weight, such as pregnancy, puts added stress on your plantar fascia.
- High Arches or Flat Feet: Extremely high or flat arches put added stress on your plantar fascia.
- Footwear: Wearing shoes with little to no arch support, especially when you already have high or flat arches, can damage your plantar fascia over time.
- Career: Careers that require you to be on your feet for extended periods can put added stress on your plantar fascia and can even cause micro-tears.
Non-surgical Treatments for Plantar Fasciitis


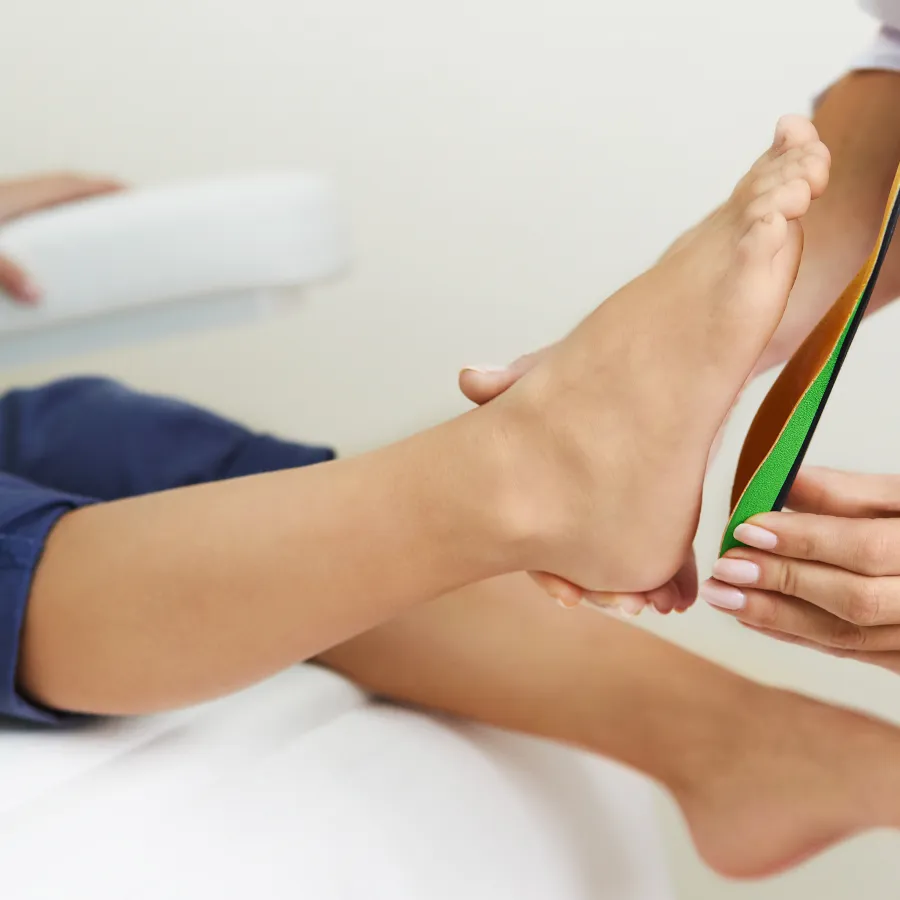
Physical Therapy
Night Splints
Orthotics
Steroids
Am I a good candidate for plantar fasciitis release surgery?
Surgery is considered a last resort, but sometimes it can be necessary. You may be a good candidate for this surgery if:
- You still suffer from chronic foot and heel pain after trying other non-invasive methods.
- Your pain has lasted for over six months while trying other, more conservative treatments.
- Your pain is affecting your ability to perform daily activities and exercises.
- Your pain is affecting the way you walk.
- Your pain is interfering with your ability to work.
- You do not suffer from underlying health issues such as diabetes.
Surgery Aftercare
Your post-op instructions will depend on which type of surgery you had. For both types, your doctor may prescribe you pain medications or recommend over-the-counter meds.

Open Surgery Recovery
You may be required to wear a special shoe or walking boot for several weeks after your surgery. This helps your foot stay protected while it heals and alleviates the weight from walking. You will have a small scar where the 1-2 inch incision was made after the sutures are removed. You can begin wearing normal shoes when your doctor gives the ok, but full recovery typically takes between 6-10 weeks.

Endoscopic Surgery Recovery
This type has a quicker recovery period and you should be able to bear limited weight almost immediately after surgery. Rather than being put in a cast or a boot, you can wear regular shoes within 1-2 days post-operation. Since the incisions are less than half an inch long, your scars will be very small. You'll be advised on what activities to avoid following your surgery, but full recovery typically only takes between 3-6 weeks.
Heel Spur vs. Plantar Fasciitis
Heel spurs and plantar fasciitis can be difficult to tell apart. Both cause pain in the same area, so it is important to get your heel pain checked by a board-certified orthopaedic doctor.